I had a great experience, the staff are super nice and very informative. They made sure i was fine and asked if i had any questions, the surgery itself went perfectly smooth. I would recommend them to anyone needing oral surgery. Definitely had a positive experience.
TMJ Pain That Just Won’t Go Away? We Can Help.

The temporomandibular joint (TMJ) is a small hinge with a big job—helping you talk, chew, and move your jaw comfortably. But when something goes wrong, it can lead to daily pain, clicking, locking, or trouble opening your mouth.
If conservative treatments like splints, massage, or medications haven’t helped, it may be time to explore more advanced options. At Airdrie Oral Surgery, we offer surgical and minimally invasive treatments designed to relieve stubborn TMJ symptoms and restore comfort.
What Is TMJ Disorder?
TMJ disorders are often caused by:
- Teeth grinding or clenching
- Muscle tension
- Joint damage from injury or arthritis
- Bite misalignment
Common symptoms include:
- Jaw pain or stiffness
- Clicking or popping sounds
- Headaches or facial pain
- Limited mouth opening or jaw “locking”
When Is Surgery Considered?
If non-surgical options haven’t worked—or if imaging shows clear joint damage—your oral surgeon may recommend a step-up treatment like Botox, joint flushing (arthrocentesis), or open-joint surgery.
TMJ Treatments We Provide
Botox Injections
Botox is used to relax overactive jaw muscles and reduce clenching-related pain.
- In-office procedure (10–30 minutes)
- Relief often felt within a week
- Minimal downtime
- Can be repeated as needed or used with other TMJ treatments
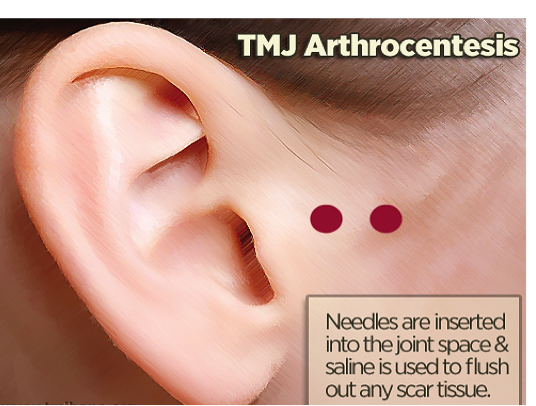
TMJ Arthrocentesis
This is a minimally invasive procedure done under anesthesia to reduce inflammation inside the joint.
- Two small needles are used to flush the joint with sterile fluid
- May include a steroid injection to reduce swelling
- Ideal for patients with joint pain, locking, or stiffness
- Same-day procedure with a short recovery time
Open Joint Surgery (Arthroplasty)
For patients with significant joint damage, open surgery may offer the best outcome.
- Removes scar tissue, bone spurs, or damaged discs
- May involve repositioning or reconstructing part of the joint
- Recommended for severe cases or when other treatments haven’t helped
- Done under general anesthesia with follow-up care
Recovery & Results
Each treatment has a different healing timeline, and we’ll guide you through every step. Our team provides custom post-op instructions and follow-up support to help ensure a smooth recovery and lasting results.
Want to Learn More?
Check out the Calgary Oral Surgery Group’s TMJ Disorders Page for additional insights into TMJ care.
Let’s Find the Right Solution
If your jaw pain isn’t improving, we’re here to help. Call Airdrie Oral Surgery to schedule a TMJ consultation and take the next step toward lasting relief.